“It’s a very methodical process,” she says, “a lot of 1-2-3 counting to make sure everybody knows which moves are being made, and we have the correct hold on the feeding tube and any IV tubing, so devices and tubes don’t get dislodged.” The biggest concern in moving patients who have COVID-19 is protecting their airways, Troiani explains, so a respiratory therapist has to be present. Watch nurses prone a patient Protecting Airways, Preventing Pressure During Proning in Coronavirus Nurses from The Johns Hopkins Hospital show how to properly prone an intubated patient. The team has been called an average of eight to 10 times each shift, Sherman says. While the prone team members have regular duties, when they are paged to help prone a patient, they spring into action. Because the physical therapists usually handle patients who are less ill, Troiani conducted training in the hospital’s simulation center, using mannequins. Within a couple of days, she had assembled a three-person prone team: two outpatient physical therapists and a MICU resource nurse. Sherman contacted the MICU and partnered with Troiani, as well as nursing managers and the Department of Physical Medicine and Rehabilitation. He was discharged from the hospital and is … doing really well,” says MICU nurse Nicole Troiani. Proning and the care that he got really is what helped him survive. “We all did not think he was going to make it. Proning three to four times made a big difference for one male patient who was intubated and heavily sedated for over a month. Hospital President Redonda Miller loved the idea - and asked Sherman to get it in place quickly. Sherman immediately thought to create a prone team, like a code team that goes to units to help manage patients in crisis. All needed to be intubated and cared for in the prone position. 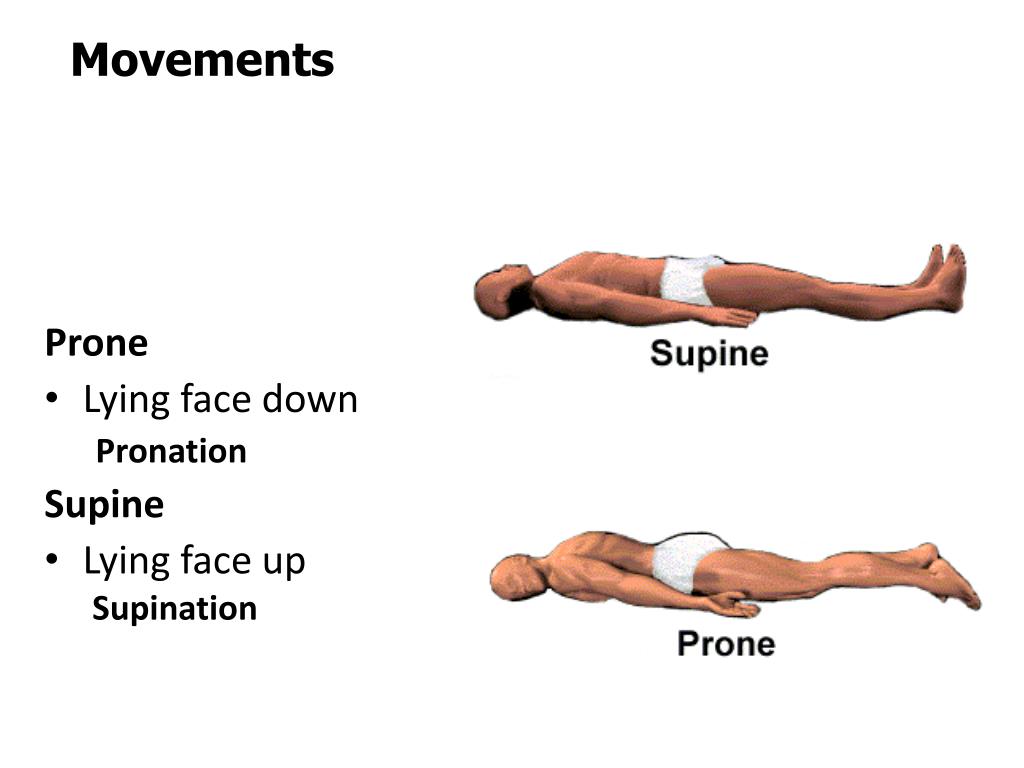
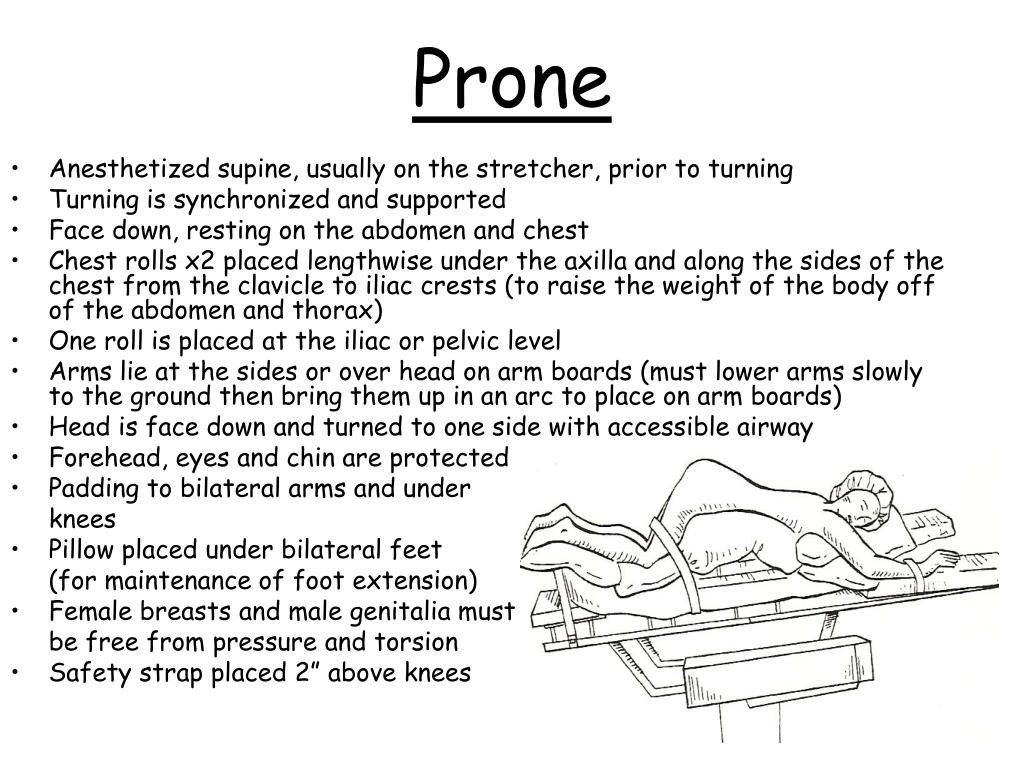
Normally, patients who need to be proned are transferred to the MICU, but with so many patients being treated, that wasn’t always an option.Īround the same time, nurse Deborah Sherman, program director for clinical informatics and deputy operations chief in The Johns Hopkins Hospital’s emergency management command, was in a meeting with hospital leadership discussing a large number of patients with COVID-19 who had been admitted overnight to a unit that typically cares for intermediate-level patients. Proning has long been used in the MICU for serious lung conditions like acute respiratory distress syndrome (ARDS), Troiani says. Called prone positioning, or proning, the technique relieves some of the pressure caused by gravity, the heart and diaphragm when lying on the back, and it can help clear respiratory secretions. Many hospitals are placing patients with COVID-19 on their stomachs as a method to try to increase the amount of oxygen to the bottom and back portions of the lungs. ‘Proning’ to Relieve Pressure on the Lungs in Coronavirus So she began developing resources, like step by step written instructions on how to move patients, as well as a video demonstration. “We have very experienced ICU nurses who had never had to do this,” says Troiani. With additional hospital units transformed to care for patients with COVID-19, and as placing patients on their stomachs during treatment became more widespread and evidence grew that the practice could help, the MICU charge and resource nurses were increasingly getting called to help educate units on how best to turn over and monitor patients on ventilators. As the number of patients with COVID-19 began to rise at The Johns Hopkins Hospital in March, medical intensive care unit (MICU) nurse Nicole Troiani found herself busier than ever - and not just caring for critically ill patients in her own unit.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
